Yes. Asthma can cause chest pain, tightness, or pressure. If you are searching “what does asthma chest pain feel like” or worrying “can asthma cause chest pain on my left side,” you are not alone. Thousands of asthma patients ask these same questions daily.
This guide explains exactly how asthma chest pain feels, when it is an emergency, and how the board-certified providers at Glow Primary Care in East Northport, NY, can help you.
What Does Asthma Chest Pain Feel Like?
Asthma chest pain is real, but it feels different from person to person. Based on patient descriptions and clinical reports, asthma-related chest pain typically falls into a few distinct categories
| Sensation | What It Feels Like | Most Likely Cause |
| Tightness or pressure | A band squeezing around your chest, or something heavy sitting on you | Airway inflammation and bronchoconstriction |
| Dull ache | A persistent, low-grade soreness deep in the chest | Hyperinflated lungs or prolonged inflammation |
| Sharp or stabbing | Brief, localized pain that worsens with deep breathing or coughing | Intercostal muscle strain (muscles between the ribs) |
| Burning sensation | A warmth or irritation behind the breastbone | Often confused with GERD (acid reflux), which is common in asthma |
Most people with asthma describe chest tightness as a heavy or squeezing sensation, not a sharp, sudden pain. This tightness can make it difficult to take a full breath and may be an early sign of an asthma episode.
Does asthma chest pain come and go?
Yes. Chest tightness or pain may:
- Appear only during an asthma attack
- Linger for hours or days after a flare-up (especially if coughing has been severe)
- Worsens with cold air, exercise, stress, or exposure to triggers like smoke or strong smells
- Improve after using a rescue inhaler (albuterol)
When chest pain is from coughing, not the lungs themselves
One of the most common causes of sharp, stabbing chest pain in asthma is intercostal muscle strain. Each cough exerts significant pressure on the ribcage. After repeated coughing (common in asthma), the small muscles between your ribs become strained or inflamed.
This feels like a sharp, localized pain on one or both sides of your chest that worsens when you cough, laugh, or take a deep breath.
Can Asthma Cause Chest Pain on One Side? (Left Side Concerns)
Yes, asthma can cause chest pain on one side, including the left side. However, the reason and the level of concern are different depending on the location and quality of the pain.
Left-sided chest pain: Asthma or heart?
Left-sided chest pain is frightening because it is the classic warning sign of a heart attack. But in asthma, left-sided pain is often benign and muscular.
| Location | Asthma-Related Cause |
| Left side only | Intercostal muscle strain from coughing or localized inflammation |
| Right side only | Less common – typically muscle strain |
| Both sides | Very common – chest tightness from airway inflammation |
Why Does Left-Sided Asthma Chest Pain happen
Muscle strain from coughing: Your intercostal muscles (between the ribs) are used every time you cough. If you have been coughing more than usual, a common asthma symptom, you can strain these muscles on one side more than the other, depending on your body mechanics.
Hyperinflated lungs: During an asthma attack, air becomes trapped in the lungs, causing them to over-expand. This pushes against the diaphragm and chest wall, sometimes producing a dull ache that can feel more prominent on one side.
Anxiety overlap: Asthma attacks are frightening. Anxiety and panic can cause chest wall muscle tension, rapid heartbeat, and a sharp, stabbing chest pain that feels very different from asthma tightness. Anxiety-related chest pain is often left-sided or central and can mimic heart attack symptoms.
The crucial distinction
Asthma left-sided chest pain is typically dull, aching, or tight, and often improves after using a rescue inhaler or resting the chest muscles.
Heart attack chest pain is often described as crushing pressure, squeezing, or heavy weight – and does NOT improve with an inhaler. It may radiate to the left arm, jaw, or back, and is often accompanied by nausea, cold sweats, or shortness of breath at rest.
Why Does Asthma Cause Chest Pain? 3 Main Mechanisms
Asthma-related chest pain comes from three distinct physiological mechanisms, sometimes overlapping.
Airway inflammation (the most common cause)
Asthma is fundamentally a disease of inflammation. When you encounter a trigger, cold air, pollen, smoke, exercise, or stress, your airways respond by:
- Swelling (inflammation)
- Tightening (bronchoconstriction)
- Producing excess mucus
This trio of responses narrows the airway passages. Your lungs must work much harder to move air in and out. The sensation of that extra work is often described as chest tightness, pressure, or a band-like squeeze. This is the most direct asthma-to-chest-pain pathway.
Hyperinflated lungs (the deep ache)
During an asthma attack, it becomes easier to breathe in than to breathe out. Air becomes trapped in the alveoli (air sacs) of the lungs. The lungs over-expand like overfilled balloons. This hyperinflation pushes upward against the diaphragm and outward against the rib cage.
The result: a deep, dull, aching pain that can feel like soreness after a hard workout. This pain is often felt on both sides, but can be more noticeable on one side depending on body position.
Cough-related muscle strain (the sharp pain)
Asthma causes coughing – sometimes severely. One study notes that “asthma often leads to chest pain that can range from a dull ache to a sharp or stabbing pain”. The sharp or stabbing quality almost always comes from muscle strain.
Each cough contracts the intercostal muscles (between the ribs) and the diaphragm with significant force. After 20–30 coughs, these small muscles become fatigued, strained, or inflamed. The pain is:
- Sharp or stabbing (not dull)
- Localized to a specific spot (often on one side)
- Worse with coughing, deep breathing, or twisting your torso
- Better with rest and gentle stretching
Key takeaway: If your chest pain is sharp and worsens when you cough or move, it is likely muscular rather than lung- or heart-related. However, always mention it to your doctor.
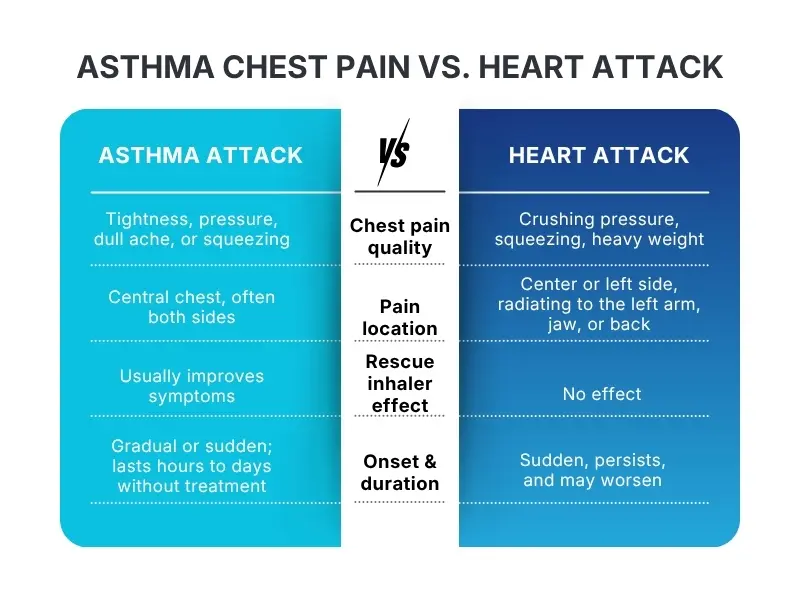
How to Tell the Difference between Asthma Chest Pain vs. Heart Attack
The table below helps you distinguish between the three.
The One Rule You Must Remember
If you are unsure whether your chest pain is asthma, a heart attack, or a panic attack, treat it as the most dangerous possibility first.
- Use your rescue inhaler.
- If the inhaler does nothing and you have crushing chest pain, nausea, cold sweats, or pain radiating to your left arm or jaw, call 911 immediately.
When to See a Doctor for Asthma Chest Pain
Use the guide below to make the right decision.
The 4-4-4 Rule (For Acute Asthma Attacks)
If you are having sudden difficulty breathing or chest tightness, follow this simple emergency first-aid method from Doctor On Demand :
4 puffs – Wait 4 minutes – Repeat 4 puffs
- Take 4 puffs from your rescue inhaler (use a spacer if available).
- Wait 4 minutes.
- If breathing has not improved, take 4 more puffs.
- If still no improvement after the second round, call 911 or go to the ER immediately.
You can repeat the 4-4-4 steps every few minutes while waiting for help, up to 20 puffs per hour maximum.
Symptoms That Require Immediate Emergency Care
Do not wait. Do not “see if it gets better.” Go to the ER or call 911 if you experience any of the following:
- Chest pain or pressure that does not improve with your rescue inhaler
- Severe wheezing when breathing in AND out
- Coughing that will not stop
- Rapid breathing that does not slow down
- Trouble talking, walking, or swallowing
- Blue, gray, or pale lips, gums, or fingernails
- “Silent chest”, no wheezing sound at all (this is a late and dangerous sign)
- Fainting, dizziness, or confusion
- Peak flow reading below 50% of your personal best after using your inhaler
What Happens If You Delay Care?
Delaying care can lead to:
- Progression to status asthmaticus (a severe, life-threatening asthma attack that does not respond to treatment)
- Respiratory failure requiring mechanical ventilation
- Permanent lung damage
- In rare cases, death
Do not guess. Do not wait. If you are worried, seek care.
When to Make an Appointment with Glow Primary Care
If your symptoms are mild, steady, or you are recovering from a flare, your primary care doctor is the right place to start. The physicians at Glow Primary Care in East Northport can:
- Adjust your maintenance medications to prevent future attacks
- Perform in-house spirometry to assess lung function
- Develop or update your personalized asthma action plan
- Identify triggers (allergy testing available)
- Coordinate care with specialists if needed
For specialized asthma care, including trigger identification and personalized treatment plans: Learn more about our asthma treatment in East Northport and how we can help you breathe easier.
References
- Cleveland Clinic. Asthma. my.clevelandclinic.org/health/diseases/6424-asthma. Published August 29, 2023.
- WebMD. Asthma. webmd.com/asthma/what-is-asthma. Originally published February 11, 2002; clinically reviewed and updated.
- Lundy C, Knox B. When to go to the Hospital for Asthma: What an ER can do for your asthma. Doctor On Demand. doctorondemand.com/blog/health/when-to-go-to-the-hospital-for-asthma/. Published October 31, 2025.
- +MEDRITE Urgent Care. Panic Attack vs Asthma Attack: Know the Difference. medriteurgentcare.com/panic-attack-vs-asthma-attack/. Published October 24, 2025.
- Pulatova KS, Jayati R, Rofeev JM. Clinical and functional characteristics of patients with chronic heart failure and bronchial asthma. Вестник Ассоциации Пульмонологов Центральной Азии. January 2026.
- Cucco A, Simpson A, Murray C, et al. Clustering lung function and symptom profiles for asthma risk stratification. Scientific Reports. 2026;16:3110.






